Israeli scientists have successfully completed a surgical operation of artificial corneal transplantation recently, which achieved a major medical breakthrough, local media reported. An old man who had been blind for ten years almost recovered his vision immediately after the operation of artificial cornea transplantation. The successful implantation of the artificial cornea is also certainly inseparable from the support of other medical research and medical device. The slit lamp has a great influence on the preoperative and postoperative examinations of this surgery.

When will keratoplasty be conducted?
Keratopathy is the most common eye disease in modern times. The lesion site of the cornea usually turns opacification and turns gray. It would hinder light from entering the eye, which can cause blurred vision, deterioration, or blindness. As per relevant statistics, approximately 2 million people go blind because of corneal problems every year.
The particularity of the cornea has led to a very low corneal donation rate. Since the mature cornea can no longer undergo cell division, corneal transplantation is the most effective way to treat keratopathy.

Development of artificial cornea
Artificial cornea refers to the vitro cultivation of transplantable corneal endothelial cell layers by artificial methods. As early as 1789, a French doctor Guillaume Pellier de Quengsy first proposed to implant a clear and thin piece of glass into the turbid cornea to restore vision. The history of keratoplasty can be traced back to 1871 when a piece of glass was first successfully implanted in a patient’s cornea.
Rabin Medical Center is at the forefront of Israel and even the world in the field of organ transplantation. In January 2021, Israel Rabin Medical Center started the clinical trial of artificial cornea transplantation with a slit lamp microscope to observe the situation in each stage and finally completed the first operation of implanting artificial cornea in the human body.
The keratoprosthesis that Israeli scientists transplanted to patients named KPro, which was developed by an Israeli technology company to treat corneal blind patients who are not suitable for traditional corneal transplantation. It is a 100% synthetic non-degradable nano-fabric skirt and being placed under the conjunctiva to replace the scarred or deformed cornea. This keratoprosthesis adopted nano-scale chemical engineering technology and made from sterile inert materials, it will not carry infectious substances or cause inflammatory reactions but can stimulate cell growth. This will improve the patient’s life quality and provide more effective care.
Although Israeli scientists have made a breakthrough in medicine, keratoplasty technology is immature and still in an experimental stage. Thereby the technology cannot be applied in clinics on a large scale currently. However, from another perspective, the success of keratoplasty sets a precedent for future practice.
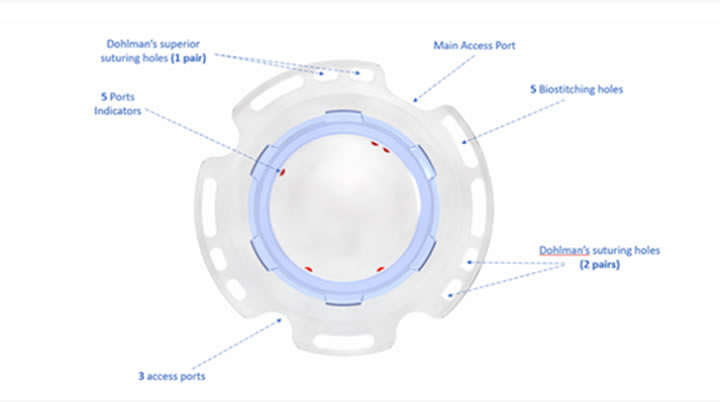
Clinical research methods of keratoplasty/artificial corneal transplantation
Clinical research must be conducted before any surgical operation. Keratoplasty has completed the preliminary clinical study, including six-month breakthrough research, which has successfully proven its safety. In January 2021, a later clinical trial has been started at Rabin Medical Center in Israel, which has been equipped with digital slit lamps and completed the first implantation in the human body.
- Firstly, implanted artificial cornea unilaterally for eligible subjects.
- A clinical follow-up started on the 1st day, 1st week, 1st, 2nd, 3rd, 6th, 9th, and 12th months after implantation. To evaluate the clinical performance of implanted artificial cornea through ophthalmic medical equipment, including slit lamp microscope, intraocular pressure measurement, and ophthalmic imaging to determine whether there is an exclusive reaction. In this stage, MediWorks’ slit lamp equipped with Mediview software assists ophthalmologists to compare multiple images on the same interface, which greatly facilitates long-term follow-up and image recording of patients.
- At the last follow-up, ophthalmologists need to use a slit lamp microscope to determine the retention rate of the artificial cornea. If going through with MediWorks’ slit lamp when doing the preoperative examination, a high-definition image with finer details can be observed.
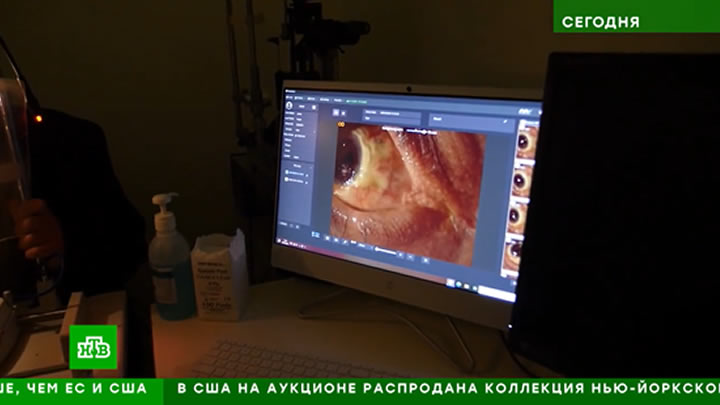
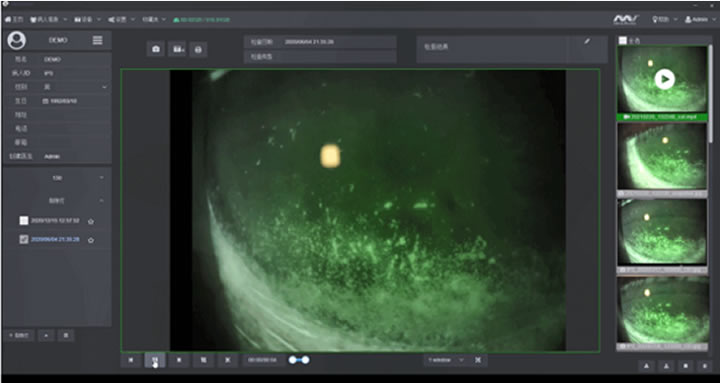
In addition, in the long-term follow-up process after the keratoplasty, if fluorescent dyeing is required, MediWorks’ slit lamp, which with the built-in yellow filter and cobalt blue light can assist clinicians in observing incision, so that clinicians can find the adverse healing condition of the incision as early as possible.
Advantages of artificial corneal transplantation
Because the artificial cornea is made from a kind of synthetic non-degradable material, once the artificial cornea is being implanted, it will stimulate the “cell proliferation” in the eyes. Thereby it can be well combined with the living tissue together and would not cause rejection in the human body. The artificial cornea and resident ocular tissue will be completely fused together over time, and the patient’s vision will get better and better. This new artificial corneal implantation is relatively simple and takes a shorter time of operation. Moreover, the surgical trauma is small and will quickly get healed after the surgery, which is able to help thousands of blind patients see again.
When the technology enters the practical stage, more people will benefit from it in the future.
Source: https://www.timesofisrael.com/haifa-resident-regains-vision-after-getting-artificial-cornea-implant/
